ulcerative colitisのムナクリ通信一覧
宗像靖彦クリニックでは、健康生活に必要なあらゆる情報発信をしております。
もっと詳しくお聞きしたい事や、他に知りたい内容などございましたら、スタッフにお伝えください。
Case ReportCase1-20202020.01.06
A 39-year-old woman presented to my clinic three years ago because of 2-year-lasting widespread muscloskeletal pain. She had visited several medical institutions including rheumatology, gynecology, and psychiatry. Blood test revealed elevation of rheumatoid factor (264 IU/mL) with no elevation of C-reactive protein. She was recommended to receive the treatment as fibromyalgia accompanied with rheumatoid arthritis at the former hospital and introduced to my clinic.
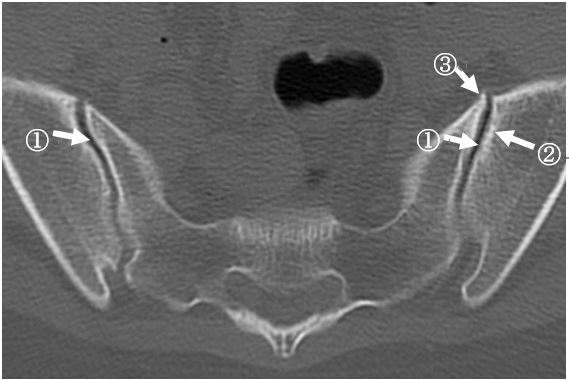
The physical examination showed sever tenderness on sacroiliac joints. There are no tender and swelling joints on fingers. Acetaminophen is partially effective for her back pain. Her symptoms are classified as inflammatory back pain. Computed tomography of sacroiliac joints showed vacumm phenomenon(①), erosion(②), and osteophyte(③). These are inappropriate findings for her age. These findings suggested the presence of sacroiliitis and/or spondyloarthtitis. She was not able to take acetaminophen continuously because of gastric adverse effects. She was treated with tramadol hydrochloride to reduce pain.
Severe diarrhea manifested itself two months ago. Total colonoscopy was performed and a diagnosis of ulcerative colitis was made. She is now treated with prednisolone and mesalazine. The widespread muscloskeletal pain including back pain is prominently relieved. She is going to be treated with bDMARD for tapering-off prednisolone.
In this case, the widespread muscloskeletal pain resembling fibromyalgia was appeared five years prior to the intestinal symptoms of ulcerative colitis. However, inflammatory back pain and age-inappropriate findings at sacroiliac joints were observed at almost same time of onset of the disease. Sacroiliitis and/or spondyloarthritis may predict the latent ulcerative colitis.
【Key Words】




